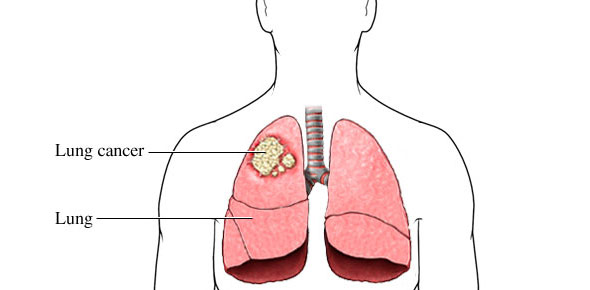
A minority of lung cancer patients present with paraneoplastic manifestations; these features may be important clues to early diagnosis and may have a bearing on treatment options. The biology of some of these syndromes remains poorly characterized, but some of the syndromes may relate to cytokine-mediated responses to antigens from the intrathoracic lung tumor, rather than the result of distant spread of cancer. The most common paraneoplastic feature associated with lung cancer is clubbing of the fingers from periosteal swelling of the distal phalanges, which may occur in 5% to 15% of patients. In a small percentage of patients, clubbing may be part of a symptomatic hypertrophic osteoarthropathy. These patients often complain of a distal symmetrical arthritis that most commonly involves the ankles or knees but can also involve the wrists, elbows, and other joints. Misdiagnosis of this condition as a strictly rheumatologic phenomenon often results in delayed recognition of the underlying neoplasm. Although weight loss and fatigue are commonly an indication of distant metastasis, they can also represent a paraneoplastic phenomenon that occasionally occurs even with early-stage tumors. Especially in patients with SCLC, paraneoplastic manifestations can also take the form of specific neurologic syndromes, such as the Lambert-Eaton syndrome. These patients present with muscle weakness caused by antibodies to the postsynaptic acetylcholine receptor of the motor end plate. A variety of peripheral neuropathies and central nervous system involvement such as subacute cerebellar degeneration or limbic encephalitis occur less commonly. Another category of neoplastic syndromes relates to aberrant hormone or peptide production by lung cancer tumor cells. The most common of these is hyponatremia secondary to the production of antidiuretic hormone. Hypercalcemia can result from tumors that secrete parathyroid hormone; Cushing syndrome can be caused by tumors that secrete adrenocorticotropic hormone. In general, these hormonal syndromes are more common in SCLC than in NSCLC, because of the neuroendocrine nature of SCLC. However, hypercalcemia can have a range of causes including both remote effects and direct interactions between tumor and bone and is much more common in NSCLC than in SCLC.